Briana RegifoSave this storySave this story
Briana RegifoSave this storySave this story
On a recent Wednesday morning in the Allure group chat, an editor shared that she had had a couple of styes on her eyelids recently, and when she wondered aloud to a friend what the culprit could be, that friend replied coolly: “Maybe you have mites.” This was not welcome news. And also perhaps not really a thing? (This friend was not an ophthalmologist of any kind.) Fifteen minutes—and many concerned responses—later, we were reporting this story.
Turns out, eye mites—referred to as Demodex mites by ophthalmologists—are really a thing, and they are likely living on your eyelashes right now. But before you panic, take a deep breath (and resist the urge to rub your eyes). Mites, even when skittering in proximity to your eyeballs, are a totally normal part of your skin’s microbiome, feeding on oil and dead skin cells inside hair follicles. They’re only a problem (causing itching and redness) when a few too many of them get together. Then you’re left with blepharitis, a.k.a. Inflammation of the eyelid.
But though an -itis can sound intense, there’s still no reason to be alarmed (or, again, to rub your eyes). To put your minds—and ours—at ease, we spoke with ophthalmologists about eye mites and how you can prevent them from stirring up trouble along your lash line.
How do eye mites cause itching and irritation?
Okay, let’s back up a minute. According to ophthalmologists, there are two species of eye mites: Demodex brevis and Demodex folliculorum. Demodex brevis lives on the oil-secreting glands along the eyelids (the meibomian glands), while Demodex folliculorum resides in the lash follicles. “By the age of about 60, 100% of adults have had Demodex on their face,” says Diane Hilal-Campo, MD, a board-certified ophthalmologist in Oakland, New Jersey. (They can also live around the hair follicles and oil glands on the nose, in the eyebrows, and elsewhere.) According to a 2022 study, 25 million of the 45 million adults who visited the eye doctor that year were diagnosed with Demodex blepharitis—that’s more than 55%.
Overgrowth of mites tends to occur with aging, altered rosacea (meibomian gland dysfunction), blepharitis, immune changes, or inadequate eyelid hygiene, according to Ashley Brissette, MD, an ophthalmologist in New York City, who also works with Clinique. “Demodex mites carry bacteria on their surface and within their digestive tract as they feed off the bacteria on the eyelids and lashes. When mite numbers increase, bacterial load increases as well, which can trigger inflammation of the eyelids and ocular surface,” adds Dr. Brissette. “The inflammation (blepharitis) we see is often a combined effect of the mites themselves, associated with bacteria, and the body’s immune response to the infestation.”
In clinical practice, doctors report Demodex blepharitis most frequently in patients who wear a lot of eye makeup and/or false lashes and who report poor eyelid hygiene, such as not thoroughly removing eye makeup or not washing their pillowcases frequently.
Quick side note: Not all cases of blepharitis are caused by mites. Blepharitis refers to any inflammation of the eyelid, which can also be the result of chronic overproduction of oil on the eyelid glands, bacterial infections, or even seborrheic dermatitis. “Blepharitis caused by overproduction of oil in those meibomian glands is commonly referred to as posterior blepharitis or meibomian gland dysfunction (MGD),” says Balvinder Bharj, OD, an optometrist in Jersey City. “It’s often more about the oil being thickened, inflammatory, or stagnant rather than the lids not being cleaned well enough.”
How does wearing eye makeup lead to Demodex blepharitis?
Your favorite tubing mascara or gel eyeliner doesn’t automatically cause Demodex blepharitis, but improper removal of eye makeup can create the conditions that allow bacteria to thrive and the amount of mites to increase. “Heavy eye makeup, especially when not thoroughly removed, can trap debris and oils at the lash base, while shared cosmetics, poor makeup brush hygiene, or infrequent replacement of mascara can also introduce additional bacteria and disrupt the natural balance,” says Dr. Brissette, who’s also seen Demodex blepharitis in her practice as a result of false lashes and lash extensions. “They make proper lid hygiene more difficult, trap debris, and create a warm, oil-rich environment where mites thrive.”
When it comes to proper cleansing, “I always recommend removing eye makeup first before washing the rest of the face. That prevents pigment and debris from spreading across the eyelids and reduces unnecessary rubbing,” says Dr. Bharj, who advises using a micellar-based eye makeup remover before cleansing your face—and again afterwards if any stubborn residue remains. “Soak a cotton pad, press it on the lid for 10 to 15 seconds to dissolve the makeup, then wipe softly downward,” says Dr. Bharj. Being gentle matters more than the product you use. “The goal is to dissolve the makeup, not aggressively rub it off,” she adds. For more precise removal, Dr. Bharj suggests going in with a Q-tip soaked in micellar water after washing to target lingering eyeliner and mascara particles. “They’re especially helpful for cleaning along the lash line where buildup tends to collect,” says Dr. Bharj.
According to Dr. Brissette, it’s not the product formulation that’s the issue, but how close the product sits to the lash follicle where Demodex mites live and feed. And waterproof formulas of mascaras, and eyeliners, as well as eye makeup with chunky glitter particles, can also be particularly difficult to remove. Dr. Bharj advises avoiding them when possible—and please skip the tight lining. “Placing eyeliner directly on the waterline can clog the meibomian [eyelid] glands, which may contribute to dryness, inflammation, and stye formation,” says Dr. Bharj, who recommends applying eyeliner just below the lash line instead. If you can’t resist tight lining, stick to formulas approved for use on the waterline, advises Dr. Brissette.
When it comes to mascara, Dr. Bharj and Dr. Campo prefer traditional formulas over tubing mascaras, which they say are more difficult to remove completely. But, regardless of the formula, Dr. Bharj notes that “once exposed to air, any tube [of mascara] becomes a breeding ground for bacteria.” So replace your mascara every three months.
How do I know if I have an overgrowth of eye mites?
Plenty of issues can cause irritated eyes, including allergies or an infection, so how can someone tell if they’ve developed blepharitis from eye mites? The only way to know for sure is to see an ophthalmologist or optometrist, says Dr. Campo. “Demodex mites are tiny. We can't see them without a microscope,” she adds.
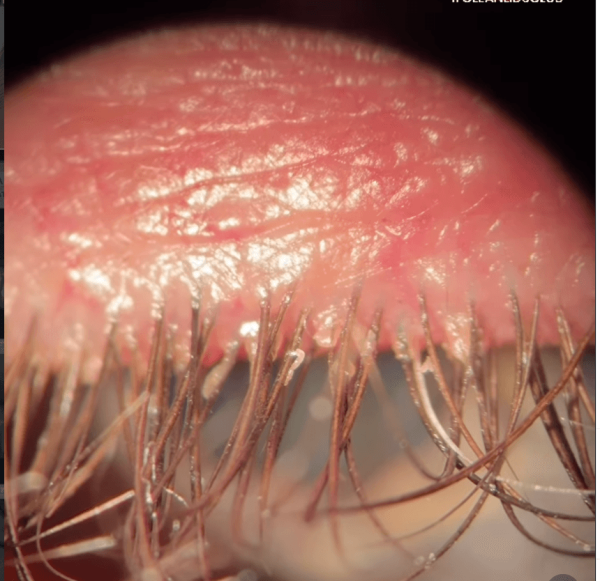
You know that part of the eye exam where you put your chin in that cradle and the doctor looks deeply (like really deeply) into your eyes with a high-intensity microscope? That slit lamp examination is what you need to properly diagnose Demodex blepharitis. During the exam, the doctor will look for collarettes—flaky, dandruff-like debris—on the lash margin. “Any amount of collarettes is indicative of Demodex,” Dr. Bharj says.
Courtesy of Dr. Balvinder Bharj, OD.
Several hallmark symptoms can suggest blepharitis before you make an appointment. “You may have eye irritation, itching along the lash line, a burning sensation, redness, crusting, flaky debris at the base of the lashes, as well as missing or misdirected eyelashes,” says Dr. Bharj. You might also get a stye, as Demodex mites can inhabit the lash follicles and burrow deep into the meibomian glands. “When these glands become inflamed or obstructed, the environment becomes ideal for blockage, and a stye is essentially a clogged oil gland, similar to a pimple,” Dr. Bharj explains. It’s essential to see an eye doctor for a proper diagnosis and treatment plan.
How to treat blepharitis caused by eye mites
To treat Demodex blepharitis, warm compresses and tea tree oil wipes are often recommended as a first-line solution. Tea tree oil kills Demodex mites, making these wipes more effective than makeup remover or micellar water. Your regular eye makeup remover may clear collarettes and keep the eyelids clean after treatment, but it won’t address the mites. Eye-care brands like Optase, Cliradex, and Belphadex make over-the-counter tea tree oil wipes specifically for Demodex overgrowth, gently removing debris, excess oil, and bacteria from the eyelids. Because the life cycle of Demodex folliculorum is approximately two to four weeks, Dr. Bharj recommends a six-week course of tea tree oil wipes to fully address any returning mites. She instructs patients to use the wipes twice daily and come back after three weeks for a recheck. “At that three-week mark, I usually see significant improvement in the mite load and symptoms,” says Dr. Bharj. Even if symptoms improve quickly, she typically advises patients to complete the full six-week course of treatment to “reduce recurrence and lingering inflammation.”
Warm compresses are also commonly recommended because heat helps liquify thickened meibum from the glands so it can be expressed more easily. “I often pair this method with a gentle lid massage,” says Dr. Bharj.
Some doctors will prescribe antibiotic ointments based on the reason for the overgrowth of Demodex, the amount of Demodex present, and the patient’s symptoms. “Prescription steroid drops or ointments are also good for treating inflammation,” says Dr. Bharj.
And if none of that works? Perhaps you’ve seen the commercials for Xdemvy, the first and only FDA-approved treatment specifically for blepharitis caused by Demodex mites. You definitely wouldn’t forget the visual of actors dressed up in mucus-hued, eight-legged costumes having a party in a patch of towering eyelashes. Dr. Campo has been prescribing the drops to treat Demodex mites and has found them to be “excellent” for those patients who don’t have luck with over-the-counter products. “You use one drop in each eye twice a day for a six-week treatment,” she says. Dr. Bharj and Dr. Campo say that after completing treatment, the mites should be eradicated.
A more aggressive option is IPL, or Intense Pulsed Light therapy, traditionally used by dermatologists to treat skin issues like rosacea. A few years ago, the FDA approved IPL to treat dry eye, and ophthalmologists have found that it can also address eyelid mites—the heat kills them, explains Dr. Campo. The FDA has not approved IPL to treat Demodex blepharitis. However, many ophthalmologists consider it to be a safe, off-label treatment, typically reserved for more severe cases where symptoms persist after over-the-counter products and prescriptions like Xdemvy have worked.
Even after treatment, maintenance is key to keeping the mites in check. The ophthalmologists we spoke with emphasized that consistent lid hygiene is the best defense against a recurrence of Demodex mites. That means thoroughly removing eye makeup every night, replacing mascara and eyeliner every three months, washing pillowcases at least once a week, and, even if you don’t wear makeup, gently cleansing the lash line with micellar water at least weekly to prevent debris and bacteria from accumulating. For patients prone to flare-ups, Dr. Bharj says incorporating lid wipes into a regular routine, even after symptoms resolve, can help keep Demodex populations in check and reduce the likelihood of future inflammation.